On this page

Care at 22–23 weeks’ gestation represents one of the greatest challenges in neonatal medicine. Across industrialized countries, policies and outcomes vary significantly, particularly at 22–23 weeks. In Japan, however, many NICUs actively resuscitate infants at this gestational age, and survival among treated infants has steadily improved over the past two decades.
Rather than a single breakthrough therapy, improved outcomes appear to reflect a bundle of coordinated practices — beginning in the delivery room and continuing through long-term follow-up. Below is an overview of selected management strategies commonly used in Japan.
Stabilization Begins at Birth: Cut Cord Milking
Umbilical cord management is the first intervention affecting hemodynamic stability [1]. While delayed cord clamping is widely recommended for preterm infants [1], intact cord milking has been associated with increased severe intraventricular hemorrhage (IVH) in infants <28 weeks’ gestation [2].
In contrast, many Japanese centers perform cut cord milking [3], in which the cord is clamped and cut, and then milked toward the infant. Although high-quality evidence in 22–23-week infants remains limited, this approach is widely adopted [4] and reflects an emphasis on immediate circulatory stabilization while avoiding intact cord milking.
Immediate Intubation and Early Surfactant
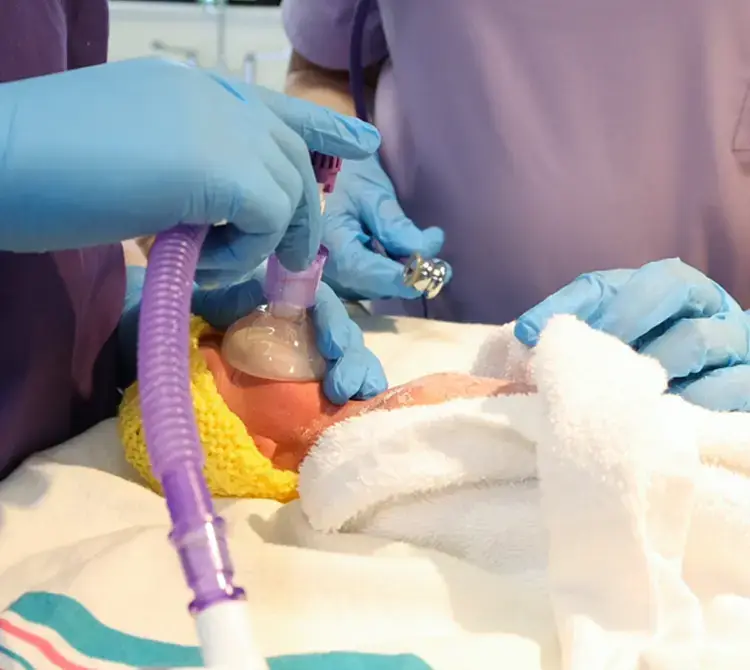
In more mature preterm infants, CPAP is often recommended as the initial respiratory strategy [5]. However, at 22–23 weeks, respiratory drive and lung compliance are profoundly immature.
Most Japanese NICUs perform immediate tracheal intubation at birth in 22–23-week infants [4]. Surfactant is frequently administered in the delivery room, often within minutes [6].
This strategy prioritizes:
- Rapid oxygenation
- Controlled ventilation
- Minimization of early physiological fluctuations
Frequent Ultrasound Monitoring: Physiology-Guided Care
- Real-time assessment of cerebral blood flow
- Early detection of hemodynamic instability
- Individualized fluid and vasoactive management
This physiology-guided model supports rapid adjustments during the most unstable phase of life.
Ventilation Strategy: From CMV to HFOV
After NICU admission, conventional mechanical ventilation (CMV) is typically used during the acute phase [3]. Once the highest IVH-risk period has passed, many centers transition to high-frequency oscillatory ventilation (HFOV) [7].
Evidence suggests HFOV may reduce bronchopulmonary dysplasia (BPD), though with an increased risk of air leaks [7]. Importantly, more recent meta-analyses do not demonstrate a significant increase in severe IVH compared with CMV [7].
The underlying philosophy is dynamic ventilation:
- Stabilize early
- Avoid large pressure fluctuations during high IVH risk
- Transition toward lung-protective strategies
Sedation During the Acute Phase
Sedation practices vary internationally, largely because high-quality evidence is limited. In Japan, some NICUs administer phenobarbital during the first days of life with the aim of reducing cerebral blood flow fluctuations and minimizing IVH risk [8].
However, systematic reviews have not demonstrated a clear protective effect against IVH [8]. This highlights an important reality in periviable care: practice variation often reflects areas of uncertainty where clinicians must balance theoretical benefit with limited evidence.
Intestinal Management: Probiotics and Routine Glycerin Enemas
Necrotizing enterocolitis (NEC) remains a major concern in extremely preterm infants.
In Japan, probiotics are used in the majority of NICUs [4], often initiated within the first few days of life and continued until later postmenstrual age. Meta-analyses support probiotic use in reducing NEC and mortality in preterm infants [9], although specific data in 22–23-week infants are sparse.
In addition, many Japanese NICUs employ routine glycerin enemas [3,4] to promote early stool passage and prevent meconium-related ileus. While systematic reviews suggest enemas improve stool frequency, they do not clearly shorten time to full feeding or reduce major morbidities. Nonetheless, the practice remains common as part of structured intestinal management.

Survival Is Not Enough
Japan reports relatively high survival among actively treated 22–23-week infants [4]. Yet long-term follow-up shows that intact survival — survival without moderate or severe neurodevelopmental impairment — remains limited.
The conversation is therefore shifting. The goal is no longer survival alone, but:
- Lung protection
- Brain protection
- Family-centered care
- Long-term neurodevelopmental support
Periviable management at 22–23 weeks is not defined by one intervention. Rather, it reflects a coordinated bundle of early stabilization, aggressive monitoring, respiratory strategy, and multidisciplinary follow-up.
As evidence continues to evolve, so too must our approach — with the ultimate aim not just of survival, but meaningful long-term outcomes.

Dr. Fumihiko Namba
Neonatologist
Professor of Pediatrics at Saitama Medical Center, Saitama Medical University
References
[1] Koo, J., Kılıçdağ, H. and Katheria, A. (2023). Umbilical cord milking-benefits and risks. Frontiers in Pediatrics, 11. doi: https://doi.org/10.3389/fped.2023.1146057.
[2] Katheria, A., Reister, F., Essers, J., Mendler, M., Hummler, H., Subramaniam, A., Carlo, W., Tita, A., Truong, G., Davis-Nelson, S., Schmölzer, G., Chari, R., Kaempf, J., Tomlinson, M., Yanowitz, T., Beck, S., Simhan, H., Dempsey, E., O’Donoghue, K. and Bhat, S. (2019). Association of Umbilical Cord Milking vs Delayed Umbilical Cord Clamping With Death or Severe Intraventricular Hemorrhage Among Preterm Infants. JAMA, [online] 322(19), pp.1877–1886. doi: https://doi.org/10.1001/jama.2019.16004
[3] Motojima, Y., Nishimura, E., Kabe, K. and Namba, F. (2023). Management and outcomes of periviable neonates born at 22 weeks of gestation: a single-center experience in Japan. Journal of Perinatology, 43(11), pp.1385–1391. doi: https://doi.org/10.1038/s41372-023-01706-4.
[4] Isayama, T., Miyakoshi, K., Namba, F., Hida, M., Morioka, I., Ishii, K., Miyashita, S., Uehara, S., Kinoshita, Y., Suga, S., Nakahata, K., Uchiyama, A. and Otsuki, K. (2024). Survival and unique clinical practices of extremely preterm infants born at 22–23 weeks’ gestation in Japan: a national survey. Archives of disease in childhood. Fetal and neonatal edition, p.fetalneonatal-326355. doi: https://doi.org/10.1136/archdischild-2023-326355.
[5] Schmolzer, G.M., Kumar, M., Pichler, G., Aziz, K., O’Reilly, M. and Cheung, P.-Y. . (2013). Non-invasive versus invasive respiratory support in preterm infants at birth: systematic review and meta-analysis. BMJ, 347(oct17 3), pp.f5980–f5980. doi: https://doi.org/10.1136/bmj.f5980.
[6] Abdel-Latif, M.E., Davis, P.G., Wheeler, K.I., De Paoli, A.G. and Dargaville, P.A. (2021). Surfactant therapy via thin catheter in preterm infants with or at risk of respiratory distress syndrome. Cochrane Database of Systematic Reviews, 2021(5). doi: https://doi.org/10.1002/14651858.cd011672.pub2.
[7] Cools, F., Offringa, M. and Askie, L.M. (2015). Elective high frequency oscillatory ventilation versus conventional ventilation for acute pulmonary dysfunction in preterm infants. Cochrane Database of Systematic Reviews, (3), CD000104. doi: https://doi.org/10.1002/14651858.cd000104.pub4.
[8] Stróżyk, A., Paraskevas, T., Romantsik, O., Grazia, M., Calevo, Banzi, R., Ley, D. and Bruschettini, M. (2023). Pharmacological pain and sedation interventions for the prevention of intraventricular hemorrhage in preterm infants on assisted ventilation – an overview of systematic reviews. Cochrane library, [online] 2023(8). doi: https://doi.org/10.1002/14651858.cd012706.pub2.
[9] Kusuda, S., Hirano, S. and Nakamura, T. (2022). Creating experiences from active treatment towards extremely preterm infants born at less than 25 weeks in Japan. Seminars in Perinatology, 46(1), p.151537. doi: https://doi.org/10.1016/j.semperi.2021.151537.